“The proactive and pervasive use of effective digital health solutions is key to progress on the path to safe, higher-quality care, just as digital solutions have been transformative in other sectors. However, the nexus between digital health and healthcare quality is complex.”
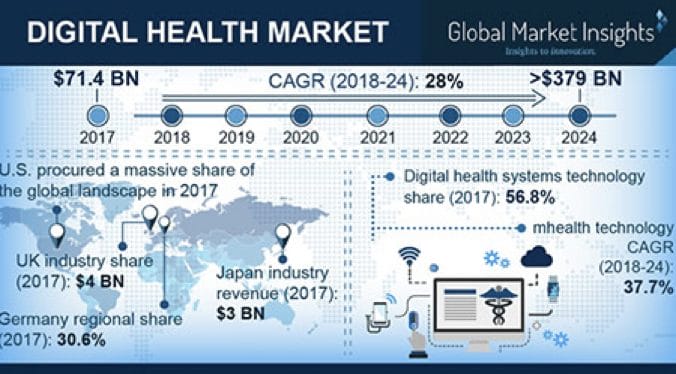
(Source: Healthcare Facilities Today)
Transformation with Digital Health
Digital health solutions geared toward providers, patients, and populations have received significant funding. In the present and the future, they serve as the cornerstone of a robust infrastructure for connected health and care.
The need for a flexible and responsive digital health ecosystem supporting resilient health systems has become apparent throughout the pandemic. For instance, regions with an existing infrastructure that could be used to track infection and immunization patterns, deliver test results promptly, or enable person-centered care with virtual care solutions were better positioned than regions without this capability.
In order to support the transformation of the healthcare system over the next ten years and beyond, there are now chances for shared learning about important facets of digital health.
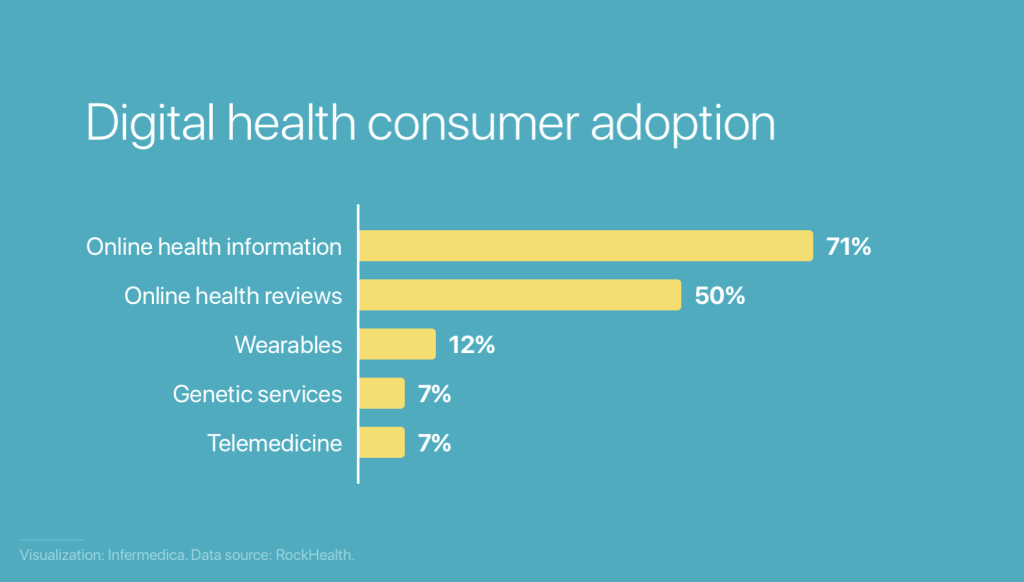
(Source: Infermedica)
Leveraging computerized decision support
Computerized decision-support systems have great potential to help clinicians process massive amounts of data and make wise decisions. Usually, these systems are placed on top of electronic health records (EHR) software. They have been used most frequently for prescription writing and medication administration. Even though there is mounting evidence to support their efficacy, problems, including inconsistent clinical impact and alert fatigue, continue to be of concern. Organizations must also invest in maintaining the underlying knowledge engines because they might quickly become outdated.

Extending care accessibility & opportunity with virtual care
Virtual modalities can execute many visits in more effective ways for both patients and clinicians, negating the need for in-person encounters in many cases. It holds true in several contexts, including intensive care and rural general care.
We have the chance to think about how to use virtual care more effectively in the future. Among the difficulties to consider are long-term adjustments in payment procedures, clinical treatment routes, and digital health literacy. It entails maximizing the blend of synchronous and asynchronous virtual care alternatives and in-person care in ways that support safety and quality.
Since virtual care has the potential to either reduce or increase health inequities, equity is another important factor. Access could be improved if people could receive care without taking as much time off from work or paying for transportation. However, lower-income, disenfranchised, and rural communities could not access broadband, which could impair their ability to get virtual care.

Shrinking gaps in public health practices
The global pandemic has revealed significant gaps in the capacity to support contemporary public health practice and adapt quickly to changing circumstances, as well as productive uses of bioinformatics and digital health by individuals, public health professionals, governments, and others.
Among the crucial uses are disease surveillance, risk communication, testing, vaccine development and distribution, and health workforce management. Utilizing pre-existing solutions has been possible in some situations, but only some of them were appropriate.

“Extending well past telehealth, McKinsey now estimates that $265 billion worth of Medicare health services could shift to the home by 2025.”
Step Into the Next Generation of Healthcare with CareCloud Wellness Suite
Innovative practices in the forthcoming wave of medical care are encouraged by CareCloud Wellness – a digital health solution. Join the industry’s groundbreaking shift from transactional to relational connection.
With our wellness suites, you can provide more outstanding care to your patients and generate higher revenue without spending more on operational resources for:
- Chronic Conditions Management (CCM)
- Remote patient observation (RPM)
Become a part of digital healthcare transformation
- Get paid more for the non-face-to-face care you already provide, such as e-prescriptions and chart reviews.
- You will promote patient engagement through regular check-ins and modifications to treatment plans.
- Operational hassles can be removed by having a devoted team to handle every activity, from the initial patient outreach to the monthly check-ins.
About CareCloud
CareCloud (Nasdaq: MTBC, MTBCO, MTBCP) brings disciplined innovation to the business of healthcare. Our suite of technology-enabled solutions helps clients increase financial and operational performance, streamline clinical workflows and improve the patient experience. More than 40,000 providers count on CareCloud to help them improve patient care while reducing administrative burdens and operating costs. Learn more about our products and services including revenue cycle management (RCM), practice management (PM), electronic health records (EHR), business intelligence, telehealth, and patient experience management (PXM) at www.carecloud.com.
The Editorial Team at Healthcare Business Today is made up of experienced healthcare writers and editors, led by managing editor Daniel Casciato, who has over 25 years of experience in healthcare journalism. Since 1998, our team has delivered trusted, high-quality health and wellness content across numerous platforms.
Disclaimer: The content on this site is for general informational purposes only and is not intended as medical, legal, or financial advice. No content published here should be construed as a substitute for professional advice, diagnosis, or treatment. Always consult with a qualified healthcare or legal professional regarding your specific needs.
See our full disclaimer for more details.







