The impact of steep declines in Medicare Advantage (MA) Star Ratings with the loss of COVID-era guardrails is already being felt by MA plans, with major plans immediately experiencing a drop in share prices when the news was released. Now, health plan leaders must act quickly to regain their footing in the next year for improved performance.
The stakes are incredibly high. Good Star Ratings yield significant benefits for MA plans, from improved enrollment to bonus payments. Low ratings put plans at a competitive disadvantage, making it harder to attract and retain members as well as offer enriched benefits. Continued poor performance can even cause termination from the MA program.
A Pivotal Moment for Medicare Advantage
Just 51% of MA plans that offer prescription-drug coverage received a four-star rating or higher when the Centers for Medicare & Medicaid Services (CMS) released the 2023 Star ratings on October 6 compared to 68% of plans a year earlier.
The achievement of such a rating is considered critical to a plan’s success in part because nearly three out of four members currently enrolled in Medicare Advantage chose a plan with a four-star or higher rating, with a coveted five-star rating representing peak performance.
Why did the ratings decrease? A new methodology for determining Star Ratings took effect for the 2023 plan year. In 2022, the methodology included measure-level adjustments that took the COVID-19 public health emergency into account. This meant that if a plan scored lower on a particular measure for the 2022 Star Ratings than it did for 2021, the plan’s measure score would revert back to the higher rating. In addition, the weight of measures around patient experience and access doubled for the 2023 ratings year.
As a result, the average Star Rating dipped from 4.37 for 2022 to 4.15 for 2023 when weighted by enrollment. According to Cotiviti’s analysis, among the 507 rated MA contracts for 2023, 9.7% earned a higher rating, 48.3% maintained their rating, and 42% earned a lower rating.
EXHIBIT ONE:
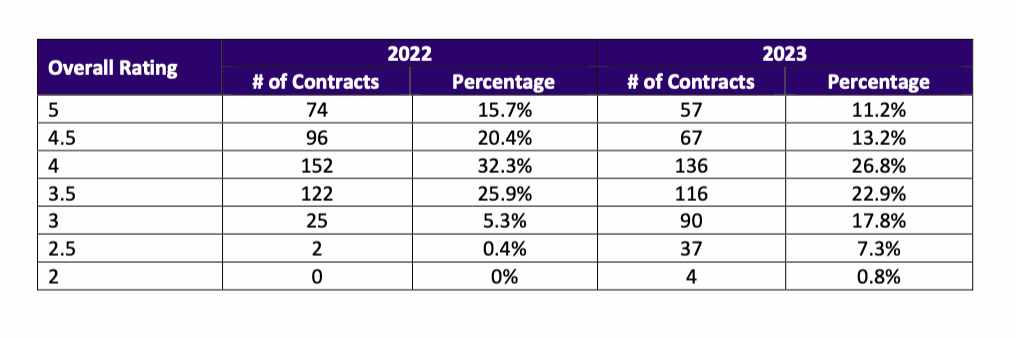
Source: Centers for Medicare & Medicaid Services data, https://www.cms.gov/newsroom/fact-sheets/2023-medicare-advantage-and-part-d-star-ratings.
Determining the Right Path Forward
How can MA plans regain their footing and drive better Star Ratings performance next year? Our experience and the experience of leading Medicare Advantage plans points to three key strategies.
- Bolster your predictive analytics capabilities. While robust reporting and dashboards are vital for tracking progress and closing gaps, MA plans need to stay one step ahead with data analytics solutions that project not only their own future performance, but also how the entire industry is trending. Such capabilities are especially important given CMS’s cut point ranges, where just one small change to a particular threshold can make or break a plan’s performance around any given measure.
Actionable intelligence based on predictive analytics will empower health plans to predict cut points as well as performance around individual measures. It will also help detect trends in performance in real time, allowing plans to make adjustments that could maintain or improve their rating in the year ahead. The right analytics solution will position MA plans to achieve their goals, whether their goal is to achieve a four-star rating or to strengthen health outcomes for a specific population. Look for a system that enables the plan to track, predict and model Star Ratings. This will help in determining the actions needed to offer better care to a growing MA population while optimizing bonus payments.
- Integrate quality measurement and reporting systems. The volume of measure sets that health plans must track and report—from Star Ratings to HEDIS® to state programs such as California’s Align Measure Perform (AMP) measure set—continues to grow. The more quality systems a health plan has in place to track and report this data, the more difficult it becomes to derive meaningful information around the steps needed to boost performance. That’s because disparate data feeds and inconsistencies in reporting make it challenging to compare information across data sources. Even within the Star Ratings program, which consists of more than 40 measures across five categories, different teams track different measures in separate locations.
By integrating their quality measurement and reporting systems, health plans can better understand their opportunities for increasing revenue and strengthening member engagement. They can also leverage more consistent reporting to drive better results with greater efficiency, eliminating the need to manage and coordinate multiple spreadsheets while reducing costs associated with ongoing maintenance and training.
- Connect quality improvement with member engagement. Given that member experience now accounts for more than half of a Medicare Advantage plan’s overall rating, health plans cannot afford to manage quality improvement and member engagement in siloes. This is especially true at a time when only 55% of Medicare Advantage members say they actively manage their care and four out of 10 say they have little to no interaction with their health plan. Plans need a multi-touch, multi-channel approach to communication that establishes trust with members—beginning with the onboarding experience—and builds a sense of collaboration in improving health outcomes and quality of life.
For example, one large not-for-profit health plan developed quality improvement triggers that alert member service agents when a member has gaps in care, such as an unfilled prescription or an unscheduled diabetic eye exam. From there, the agent can discuss any gaps in care and work with the member to proactively close them. This approach can not only improve the plan’s quality scores, but also create positive member interactions that reflect well on CAHPS survey results.
The Time Is Now
With Medicare Advantage plans experiencing widespread quality performance decreases across Star Ratings measures, health plans must have access to reliable data and data-informed intelligence to take the steps needed for improved member health and engagement and Star Ratings performance.
By making deliberate investments in predictive analytics, integrating quality measurement and reporting systems, and connecting quality improvement with multi-channel member engagement, MA plans can more effectively improve and sustain their Star Ratings. In doing so, they will create specificity in action and clarity in impact, driving better scores and continued enrollment growth amid increased expectations in a highly competitive environment.
RaeAnn Grossman is Executive Vice President of Operations for Risk Adjustment, Population Health Management and Quality, Cotiviti.
HEDIS® is a registered trademark of the National Committee for Quality Assurance (NCQA).
CAHPS® is a registered trademark of the Agency for Healthcare Research and Quality (AHRQ).








